Written and reviewed for scientific and factual accuracy by Dr. Austin Jelcick, PhD and Dr. Matthew Janzen, DC
How do scoliosis myths affect treatment and hurt our children?
There are many scoliosis myths that both doctors and patients believe; in part due to a lack of knowledge of current scientific and medical studies. Childhood scoliosis has no known cause and no cure – or so most doctors believe. As a result of this belief, when a diagnosis of scoliosis is made, little to nothing is done to try to understand or to stop the process. The standard course of action has become simply to “wait and see – observation only until surgery might be necessary.”
In practice, this means to take an X-ray in a year or so and “see” if the curve has gotten worse. If the curve progresses past 40 degrees while the child is still growing, invasive fusion surgery is prescribed. This has resulted in around 22% of kids diagnosed with scoliosis worsening in their curve size until they reach surgical range.[i] Sadly, all these scoliosis surgeries have a high complication rate.[ii]
How are we so defeated by a problem that plagues so many young adolescent spines that we have concluded we shouldn’t even try to help it? Is it acceptable to label a problem as “we don’t know” and then have a course of action which amounts to doing nothing? This is in reference to the practice of doing nothing until the problem has become so severe that the surgeon believes it necessary to perform invasive fusion surgery.
When it comes to scoliosis there, are several faulty beliefs, or myths, to which doctors and parents subscribe, and those beliefs may be hurting our children. Consider some of these accepted “truths” about adolescent idiopathic scoliosis:
Myths About Adolescent Idiopathic Scoliosis
- There is no (known) cause. Traditional medical rationale is that if there is no obvious neurological disorder, no obvious genetic disorder, and the child was not born with it, then the scoliosis is considered “idiopathic.” Unfortunately, this leads doctors to think and behave as if it cannot be known what is causing scoliosis once it is labeled “idiopathic”. The search for the diagnosis ends abruptly. It is as if we are saying “now that the scoliosis has been labeled idiopathic, that’s our final diagnosis”. But is it really?
- There is no cure. This can easily lead to the mentality that “nothing will help, so why try.”
- It will probably be okay. Since there is no cure, the best action is to console the parents and encourage them not to worry about the fact that it could get worse and need a highly invasive surgery. In actuality, however, there is a high probability of scoliosis getting worse with growth.
- Only surgery helps scoliosis. Many believe there is nothing that can be done for the problem except surgery. This results in physicians simply “waiting” until the child’s spine is bad enough to need surgery. A self-fulfilling prophecy has occurred, in which we began with the idea that “nothing will help except surgery,” so nothing is done to help until the scoliosis is bad enough to need surgery.
- Scoliosis braces aren’t that reliable for solving the problem. The belief that braces really don’t do all that much often results in a half-hearted effort in the making of a brace. Little attention is paid to details of the brace design, or to how well the brace is actually correcting the spine.
- It is necessary to radiate the child with X-rays in order to accurately assess the child’s scoliosis. Because X-rays are harmful, this results in a failure to watch the scoliosis closely enough and leads to the “X-ray once a year” practice. The truth is that standing MRI can eliminate the need for X-rays to monitor scoliosis.
- Once a year* spinal X-rays are effective to “watch” scoliosis – to assess if it is getting worse. In actuality, a child’s scoliosis can progress in rapid, sudden spurts, just like their growth. Just like a child can grow an inch in a summer, so can their scoliosis worsen that fast as well. (Some say 6 months but what we observe happening more often in practice is once a year). You can observe the problem with observing scoliosis infrequently below.
- Exercises don’t help scoliosis. Therefore don’t try.
Myths About Scoliosis: Semi Annual X-rays Are Sufficient for Monitoring
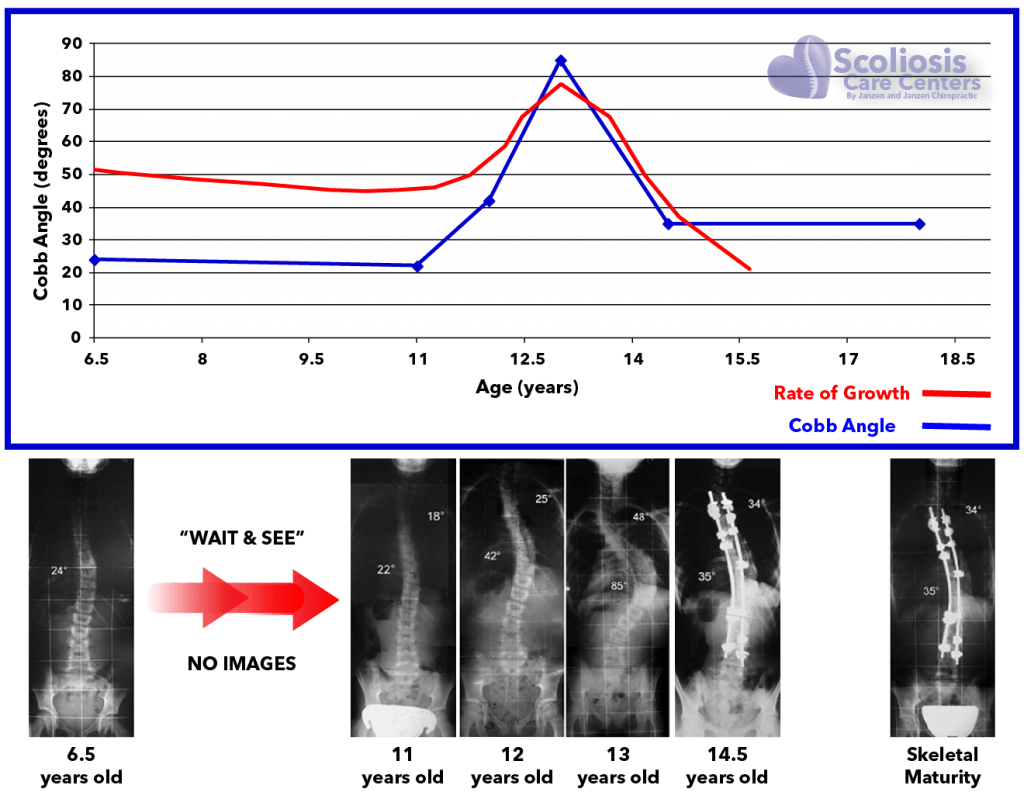
Imaging a scoliosis every ~6 months via x-ray may avoid x-ray exposure, but it can easily miss a rapid progression. Because scoliosis progresses relative to how fast a child grows, a curve can worsen very quickly during a growth spurt during puberty. This rapid worsening (and the ideal window for correction) can be easily missed if we only examine the spine every 6-12 months. Using radiation-free imaging methods such as MRI allows us to check the spine frequently, detect trouble, and intervene to straighten the spine.
It is the author’s opinion that ALL of the above beliefs are false, and they result in a major error in the way our children with scoliosis are being cared for.
The worst thing that can be done for a child with scoliosis is to do nothing. Watching the spine once a year is rarely often enough to prevent scoliosis from growing uncontrollably worse, resulting in spinal fusion. When science has shown that a child’s scoliosis can rapidly worsen during their growth spurt, and that non-surgical treatment is more successful the earlier it is performed (while the child is skeletally immature and before structural changes to the spine occur), it is easy to see that there are a large number of scoliosis myths out there which contradict published scientific studies.
There is a better way – a much better way. It begins with understanding the truth and known data about scoliosis. Scoliosis, like many problems, DOES have a cause, and that this cause may be known, and it may be treated. Your child’s spine can indeed be reliably, predictably, and effectively treated in a way that virtually assures the avoidance of surgical fusion. Just don’t wait until it’s too late; Take action now – the moment you learn of your child’s scoliosis, and allow us to help!
References
- Dolan LA, Weinstein SL. Surgical rates after observation and bracing for adolescent idiopathic scoliosis: an evidence-based review. Spine (Phila Pa 1976) 2007;32: S91-S100.
- Weiss H-R, Goodall D. Rate of complications in scoliosis surgery – a systematic review of the Pub Med literature. Scoliosis 2008 Aug 5;3:9. doi: 10.1186/1748-7161-3-9.

